At a glance
- STEP 9 (Bliddal et al., NEJM 2024, PMID 39476339) reported a 13.7% mean weight loss and a 41.7-point WOMAC pain reduction at 68 weeks on semaglutide 2.4 mg, versus 3.2% and 27.5 points on placebo
- Liraglutide 3 mg in a 2021 RCT (Gudbergsen et al., PMID 33471039) added weight loss but no extra knee pain reduction after an 8-week diet run-in, suggesting magnitude of weight loss is the lever
- A 2026 Cell Metabolism paper (Qin et al., PMID 41666927) showed semaglutide protects cartilage in pair-fed mice via the GLP-1R/AMPK/PFKFB3 axis, supporting a weight-loss-independent mechanism
- Shanghai Osteoarthritis Cohort (Zhu et al., Ann Rheum Dis 2023, PMID 37258065) tied GLP-1RA use in T2D-OA to fewer knee surgeries (1.7% vs 5.9%) and slower medial cartilage loss
- Semaglutide is not FDA approved for knee OA; STEP 9 supports a label-expansion case but everyday use is still off-label, weight-management-indicated
A Phase 3 trial built on knees, not BMI lines
For two decades, knee osteoarthritis in obese adults has been treated mostly as a weight problem with a joint complication. STEP 9 changed the framing. In a 68-week Phase 3 trial of 407 adults with BMI at or above 30 and Kellgren-Lawrence grade 2 or 3 knee osteoarthritis, weekly subcutaneous semaglutide at 2.4 mg produced a mean 13.7% weight reduction and a 41.7-point drop in WOMAC pain at 68 weeks. Placebo arm: 3.2% weight loss and a 27.5-point WOMAC pain drop. Both primary endpoints hit p < 0.001 (Bliddal et al., NEJM 2024).
The headline number is the WOMAC pain delta. A 14-point improvement over an already-active placebo arm, on a 0-to-100 pain scale and a knee OA population with a mean baseline pain score of 70.9, is the largest pain reduction shown by any pharmacologic weight-loss agent in a randomized OA trial to date. The SF-36 physical-function delta (12.0 vs 6.5 points) sits on top of that, and physical-function scores typically move less than pain in OA trials.
This article walks through what STEP 9 actually showed, why the older liraglutide knee OA trial did not show the same thing, what the 2026 Cell Metabolism paper on chondrocyte metabolism added to the conversation, and where this leaves a researcher or patient thinking about GLP-1 receptor agonists and joint disease.
STEP 9 in numbers, not adjectives
STEP 9 (NCT05064735) enrolled at 61 sites in 11 countries. Inclusion required:
- BMI 30 or higher
- Clinically diagnosed knee OA
- Kellgren-Lawrence radiographic grade 2 or 3
- WOMAC pain score 40 or higher at screening (moderate-to-severe pain)
- Stable analgesic use
Participants were randomized 2:1 to semaglutide 2.4 mg weekly or placebo, both arms received counseling on a reduced-calorie diet and physical activity. Mean age 56, mean BMI 40.3, mean baseline WOMAC pain 70.9. The two co-primary endpoints were percent body weight change and WOMAC pain change at week 68.
| Endpoint at week 68 | Semaglutide 2.4 mg | Placebo | Estimated difference | p-value |
|---|---|---|---|---|
| Body weight change | -13.7% | -3.2% | -10.5 pp | <0.001 |
| WOMAC pain (0-100) | -41.7 pts | -27.5 pts | -14.1 pts | <0.001 |
| SF-36 physical function | +12.0 pts | +6.5 pts | +5.4 pts | <0.001 |
Two things stand out beyond the headline.
First, the placebo arm dropped 27.5 WOMAC points. That is a large placebo response, which is normal in OA trials, and it makes the active-arm effect harder to manufacture by chance. Second, the subgroup analyses showed pain improvement in all BMI strata. The BMI 35-to-40 group had slightly less pain reduction than the BMI 40 or higher group. The implication is not "more BMI to lose means more pain to lose," which would be the cleanest weight-loss-only story. It is messier, which matters for the mechanism question below.
Bottom line: STEP 9 is the first Phase 3 pharmacology trial in obese knee OA to clear the WOMAC pain threshold typically used as a disease-modifying signal, with a 14-point placebo-adjusted effect at 68 weeks.
The liraglutide trial that almost everyone forgets
Before STEP 9, the only randomized GLP-1 trial in knee OA was a 2021 liraglutide study from the Frederiksberg group (Gudbergsen et al., Am J Clin Nutr 2021). The design was clever and the result was sobering. All 156 participants first lost more than 5% of body weight on an 8-week low-calorie diet, then were randomized to liraglutide 3 mg daily or placebo for 52 weeks.
Liraglutide produced an additional 2.8 kg of weight loss versus a 1.2 kg regain in placebo. But the KOOS pain endpoint did not move: 0.4 points in the liraglutide group and -0.6 in placebo, with no group difference. Most people read this and conclude that GLP-1 agonists do not help OA pain. The cleaner reading is narrower: a modest additional weight loss (3.9 kg group difference) on top of an already-completed diet does not produce a measurable additional pain reduction.
STEP 9 differs in three ways that probably matter:
- Magnitude of weight loss. Semaglutide 2.4 mg produced 13.7% from a baseline of 40.3 BMI. That is roughly 13 to 14 kg, not 4 kg.
- Trial design. No pre-randomization diet run-in. The full effect was captured.
- Drug. Semaglutide and liraglutide are not interchangeable. Both engage GLP-1R but at very different total exposures over a dosing interval, and the high-dose semaglutide regimen produces sustained receptor activation that liraglutide 3 mg daily does not match.
The 2024 retrospective cohort analysis of US claims data covering 39,394 GLP-1-treated obese adults reinforced the drug-specific pattern. Adjusted OA risk over six months was 27% lower in GLP-1 users versus non-users (HR 0.73, 95% CI 0.67-0.79). Within the GLP-1 class, tirzepatide had a lower OA hazard than semaglutide (HR 0.57, 95% CI 0.50-0.65), and liraglutide had a higher hazard than tirzepatide (HR 1.63, 95% CI 1.23-2.15) (Hong et al., Expert Opin Pharmacother 2024). Claims data are not Phase 3 outcomes, but the gradient across agents tracks expected weight-loss magnitude and gives a real-world reading consistent with what STEP 9 produced experimentally.
The mechanism question: just weight loss, or something more?
The honest 2024 answer to "how does semaglutide help OA" was: probably mostly weight loss, with a possible direct anti-inflammatory component nobody had isolated yet. The 2026 answer is more interesting.
A March 2026 paper in Cell Metabolism designed an obese mouse OA model with a pair-fed control arm. Pair-fed mice ate the same restricted calories as semaglutide-treated mice and lost the same amount of weight, without getting the drug. Semaglutide-treated mice showed reduced cartilage degeneration, fewer osteophytes, less synovial pathology, and lower pain sensitivity. Pair-fed mice did not get the cartilage benefit. The weight-loss-only arm reproduced the metabolic shift but not the joint protection (Qin et al., Cell Metabolism 2026).
Mechanistically, the group traced the chondrocyte effect to the GLP-1R/AMPK/PFKFB3 axis. Under inflammatory conditions, OA chondrocytes default to glycolysis (2 ATP per glucose) which fuels catabolic enzyme expression. Semaglutide treatment shifted the chondrocyte metabolic profile toward oxidative phosphorylation (up to 36 ATP per glucose) by suppressing PFKFB3 downstream of AMPK activation. Lower glycolytic flux tracked with lower IL-6 and TNF-alpha in the joint and with preserved type II collagen and aggrecan.
The clinical arm of the same paper was small but directional. Twenty obese adults aged 50 to 75 with knee OA received either sodium hyaluronate alone or sodium hyaluronate plus semaglutide for 24 weeks. The combination arm had lower pain scores and, on MRI, thicker cartilage in weight-bearing regions of the medial femur. This is a 20-person pilot, not a Phase 3 readout, and the trial design cannot fully separate weight-loss from non-weight-loss contributions in humans. But it is consistent with the preclinical signal.
Earlier preclinical work supports the same direction. Meurot et al., Scientific Reports 2022 showed intra-articular liraglutide reduced pain behavior in a sodium monoiodoacetate mouse OA model, suppressed IL-6, PGE2, and nitric oxide in chondrocytes and macrophages, shifted macrophage polarization from M1 to M2, and lowered MMP and aggrecanase activity. Different drug, different administration route, same direction of effect.
What the Shanghai cohort added: surgery rates and cartilage MRI
The Shanghai Osteoarthritis Cohort study sat between preclinical mechanism and Phase 3 efficacy. It analyzed 1,807 patients with both knee OA and type 2 diabetes, 233 on a GLP-1 receptor agonist and 1,574 not. Over a median follow-up of about 4 years, the GLP-1 group had (Zhu et al., Ann Rheum Dis 2023):
- Greater weight loss (-7.29 kg)
- Lower incidence of knee surgery (1.7% vs 5.9%)
- Larger WOMAC pain and total improvements
- Slower cartilage-loss velocity in the medial femorotibial compartment on MRI
The MRI signal is the part most often missed in the popular coverage. WOMAC pain is subjective. Knee surgery is a downstream event with many confounders. Cartilage loss velocity is a structural endpoint that approximates disease-modifying activity. The Shanghai group's finding that GLP-1 use tracked with slower cartilage thinning, mediated by weight loss but not fully explained by it, lined up with what STEP 9 and the Cell Metabolism paper later showed in different ways.
A 2025 review in Pharmacotherapy summarized the cumulative case across these strands and concluded that the GLP-1 class has a credible disease-modifying signal in knee OA, contingent on sustained weight loss in obese populations and possibly extending beyond that subgroup if the chondrocyte-metabolic mechanism holds up in larger human trials (Ryan et al., Pharmacotherapy 2025).
How this stacks against other GLP-1 indication expansions
Semaglutide's indication map in 2026 looks very different from 2022. The same molecule that started as a type 2 diabetes drug has moved through cardiovascular outcomes (SELECT), chronic kidney disease (FLOW), MASH (ESSENCE), Alzheimer's (EVOKE), Parkinson's, and now knee OA. Each of those readouts is a real Phase 3 dataset with different mechanism stories and different label implications.
| Indication | Trial | Year | Primary result | Label status (May 2026) |
|---|---|---|---|---|
| Type 2 diabetes | SUSTAIN-6 | 2016 | CV benefit | Approved (Ozempic) |
| Weight management | STEP 1 | 2021 | 14.9% weight loss | Approved (Wegovy) |
| CV outcomes in obesity | SELECT | 2023 | 20% MACE reduction | Approved CV indication |
| HFpEF + obesity | STEP HFpEF | 2023 | KCCQ-CSS improved | Off-label use only |
| CKD in T2D | FLOW | 2024 | 24% kidney composite | Indication filed |
| Knee OA + obesity | STEP 9 | 2024 | -41.7 WOMAC pts | Not approved, off-label |
| MASH | ESSENCE | 2024-2025 | Fibrosis improvement | Indication filed |
| Early Alzheimer's | EVOKE / EVOKE+ | 2025 | Did not meet primary | No indication |
Note: STEP 9 has been submitted to FDA as part of a label expansion case. As of May 2026 there is no separate OA indication. Wegovy is prescribed for OA pain only via the existing weight-management label, which is how almost all current real-world use is captured.
Tirzepatide has its own OA story coming. The SURMOUNT-OA trial is in the design phase, and the dual GIP/GLP-1 mechanism plus the larger weight-loss magnitude (about 22.5% at 15 mg in SURMOUNT-1) make the expected effect size in OA at least as strong as semaglutide's. The retrospective claims data already suggest tirzepatide tracks with the lowest OA hazard in the class. The Phase 3 randomized confirmation is the missing piece.
Practical reading for someone with knee OA and obesity
A few specific takeaways from the evidence base, framed for someone thinking about whether semaglutide is a reasonable part of their joint-pain plan.
Weight loss has to be real. The liraglutide trial result was not a class failure. It showed that an extra 4 kg on top of an 8% diet-induced loss does not move pain further. The STEP 9 result was a 13.7% loss in people who entered the trial obese. If a semaglutide protocol is producing 2 to 4% weight loss because of dose, titration, or adherence problems, the OA pain effect will look much closer to the liraglutide trial than to STEP 9.
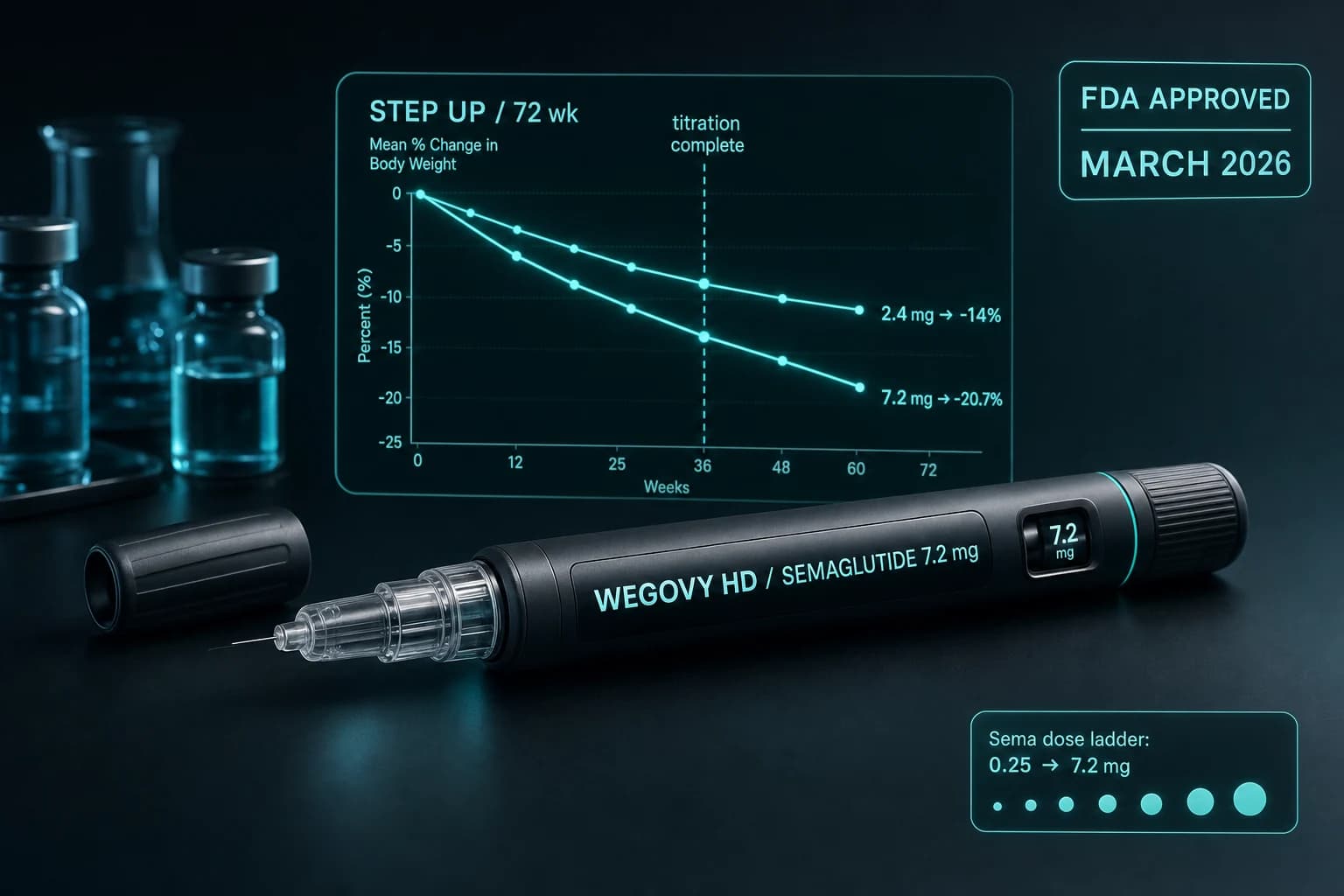
Dose matters and titration matters. The high-dose semaglutide regimen (2.4 mg weekly via Wegovy or the new Wegovy HD 7.2 mg approved in March 2026) is what was studied. Lower diabetes-dose semaglutide (Ozempic 1.0 mg) was not. The drug, the dose, and the titration protocol are part of the STEP 9 result, not optional.
Sustained effect requires sustained use. Stopping a GLP-1 typically produces weight regain. For an OA pain endpoint, regaining weight should be expected to bring back some portion of the pain. The chondrocyte metabolic story in the 2026 paper suggests there may be a residual structural benefit from time on treatment, but that has not been tested directly in humans.
Muscle loss complicates the picture. GLP-1-mediated weight loss carries a lean-mass cost that matters for joint biomechanics. Resistance training and protein intake during weight loss are not a sidebar in an OA context, they are central. The functional benefit on SF-36 in STEP 9 happened despite this, which is informative. Adding deliberate lean-mass preservation strategies should at minimum not hurt.
Safety profile is the standard semaglutide profile. In STEP 9, discontinuation for adverse events occurred in 6.7% of the semaglutide arm versus 3.0% of placebo, with gastrointestinal disorders being the primary driver. Serious adverse events were similar between arms. The OA population added no novel safety signal beyond what STEP 1-8 already established for semaglutide 2.4 mg.
Warning: STEP 9 was a 68-week trial in obese adults with radiographic knee OA. The result does not extrapolate to non-obese OA, isolated hip OA, post-traumatic OA, or short-term courses. Off-label use specifically for OA pain in a non-obese patient is not supported by these data.
How knee OA fits into the broader weight-loss-plus-comorbidity picture
The pattern across SELECT, FLOW, SUMMIT, STEP-HFpEF, ESSENCE, and STEP 9 is consistent. Sustained weight loss in obese adults with a comorbid metabolic disease produces meaningful end-organ benefit that is larger than the weight loss alone would predict. CKD progression, MACE, HFpEF symptoms, MASH fibrosis, OA pain. The disease-specific mechanisms differ, but the rough shape of the curve is the same.
This is the structural reason researchers and clinicians are gradually treating semaglutide and tirzepatide less like obesity drugs and more like multi-system metabolic agents that happen to also reduce body weight. The OA result fits the same template. The Cell Metabolism paper just gave the chondrocyte-specific mechanism that the framework needed.
For research access, semaglutide is sold by reputable vendors under research-use labeling. Limitless Biotech offers oral semaglutide analog research formulations with code ENHANCED, and injectable semaglutide for laboratory-research purposes is available from Ascension Peptides with code ENHANCED for 50% off. Clinical care belongs with a prescriber regardless of vendor channel.
What the evidence actually supports, and what it does not
It supports:
- Semaglutide 2.4 mg weekly produces a clinically meaningful pain reduction in obese adults with moderate-severe knee OA over 68 weeks
- The magnitude of pain reduction exceeds what placebo plus diet counseling delivers
- The effect is at least partly weight-loss mediated and likely partly direct via chondrocyte metabolism
- The class effect is real but agent-specific, with higher-magnitude weight-loss agents producing larger OA benefits
It does not support:
- Use in non-obese OA
- Replacing surgery for advanced disease (the trial enrolled K-L grade 2 or 3, not grade 4)
- Stopping concurrent OA management (physiotherapy, weight-bearing exercise, intra-articular interventions)
- A regulatory claim of cartilage regeneration in humans
References used in this article
- Bliddal H, et al. Once-Weekly Semaglutide in Persons with Obesity and Knee Osteoarthritis. N Engl J Med. 2024;391(17):1573-1583. PMID 39476339
- Gudbergsen H, et al. Liraglutide after diet-induced weight loss for pain and weight control in knee osteoarthritis: a randomized controlled trial. Am J Clin Nutr. 2021;113(2):314-323. PMID 33471039
- Meurot C, et al. Liraglutide, a glucagon-like peptide 1 receptor agonist, exerts analgesic, anti-inflammatory and anti-degradative actions in osteoarthritis. Sci Rep. 2022;12(1):1567. PMID 35091584
- Qin Y, et al. Semaglutide ameliorates osteoarthritis progression through a weight loss-independent metabolic restoration mechanism. Cell Metab. 2026. PMID 41666927
- Zhu H, et al. Glucagon-like peptide-1 receptor agonists as a disease-modifying therapy for knee osteoarthritis mediated by weight loss: findings from the Shanghai Osteoarthritis Cohort. Ann Rheum Dis. 2023;82(9):1218-1226. PMID 37258065
- Hong J, et al. The impact of approved anti-obesity medications on osteoarthritis. Expert Opin Pharmacother. 2024;25(11):1389-1402. PMID 39129529
- Ryan E, et al. The potential role of GLP-1 receptor agonists in osteoarthritis. Pharmacotherapy. 2025. PMID 39980227
This article is for educational and research purposes only. None of the content above constitutes medical advice. Semaglutide is FDA approved as Ozempic for type 2 diabetes, as Wegovy for chronic weight management, and as Rybelsus for type 2 diabetes. It is not approved for knee osteoarthritis. Decisions about osteoarthritis care belong with the patient and their treating clinician.